Sports Injuries and Management
Diagnosing Running Stress Fractures
The Symptoms Of A Running Stress Fracture
There are no hard and fast rules for what running stress fractures will feel like, however below are a few guidelines regarding some of the commonly mentioned symptoms of a stress fracture:
- Although most develop gradually, running stress fractures often come on without warning and frequently there is no obvious explanation for the onset of pain, meaning there is no history of trauma, or injury occurring to trigger the onset of pain.
- Don’t be fooled into thinking that you only have a stress fracture if you are unable to run due to pain. Early on in the life of a stress fracture people can often run through the pain. However a guide can be that if it doesn’t feel better as a run progresses, it can be a sign of a stress fracture. Unlike many tendinopathy complaints that can appear to loosen during a run, starting off stiff and “freeing up” as the run progress, a stress fracture running not always, but typically do not get better through the run, they commonly get progressively more uncomfortable. Eventually as with many injuries the progression of a stress fractures is that they can end up hurting not just during, or after running, but whilst walking, or even when non-weightbearing.
- Running stress fractures generally feel like an aching, or burning sensation localised somewhere along the bone. If the stress fracture is on a long bone like the tibia, or femur where there is a lot of muscle tissue around the site of injury, then these muscles may also feel very tight, another reason that making a diagnosis of a stress fracture can be challenging as the athlete will frequently report that they think it is a muscular pain.
- Usually, palpating the are will provoke pain, meaning you may be able to find a spot on the bone where pressure on that area will produce exquisite pain.
If you suspect you have a running stress fracture, then the immediate advice would be that you should stop running immediately and seek professional opinion via your physiotherapist, GP, or sports medicine specialist as soon as possible.
Diagnostic Tests
Clinical tests such as palpation of the area and the “hop test” (which means it hurts if you are hopping on the injured leg) can be coupled with a detailed history of training loads and pain presentation to help diagnose a stress fracture. However for certainty and grading the severity then investigations are extremely beneficial.
If you suspect you have a stress fracture, then some tests that can be ordered to help confirm the diagnosis include:
- Traditional X-rays: X-rays often are not sensitive enough to pick up running stress fractures, at least not in the early stages. With chronic stress fractures, or healing stress fractures an X-ray may identify the evidence of healing at the site of injury, but in the initial stages of injury using them to obtain a diagnosis X-rays are often of little use.
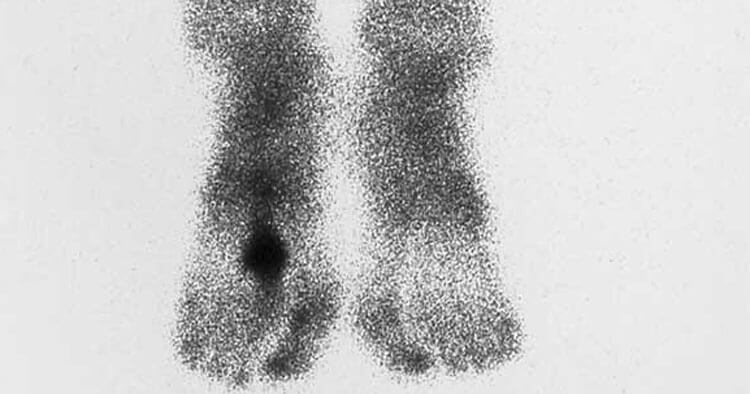
- The use of MRI, or bone scans are both considerably more sensitive at assessing and diagnosing stress fractures, as a result MRI and bone scans are preferred over plain X-rays. Bone scans when correlated with the clinical history are an accurate and reliable way to identify the presence of a stress fracture, however MRI is better when wanting to get an idea of the severity and estimate return to running time frames as well as this an MRI gives more information about any surrounding soft tissue changes.
Tip: If you have fairly recently changed your training load and have pain when running focused around one area of the bone and this pain becomes constant, or worse during a run, then you should stop training and see your physiotherapist or sports medicine specialist immediately. As these signs indicate that there is a good chance that you may have developed a stress reaction in the bone.
Picking up a bone reaction early on is crucial. Sometimes if caught early on there may simply be a stress reaction of the bone and things have not progressed to being an actual stress fracture. Conversely, running through the pain of a bone stress reaction may cause the progression to a more significant stress fracture in the bone, or even a complete bone fracture.
If you manage to catch a running stress fracture early on in the stress reaction stage, which is likely if you stop immediately at the onset of any symptoms, then this may only require you to have a mere few weeks off training. Where as pushing through the pain associated with a stress fracture, continuing to train, or run could lead to a complete fracture of the bone, meaning a significant time away from running, somewhere in the realm of several months load management being required.
Disclaimer: Sydney Physio Clinic provides this information as an educational service and is not intended to serve as medical advice. Anyone seeking specific advice or assistance on Diagnosing Running Stress Fractures should consult his or her general practitioner, physiotherapist, sports medicine specialist, orthopedic surgeon or otherwise appropriately skilled practitioner.