Injury Rehabilitation and Training, Muscle Pain and Tendinopathy, Sports Injuries and Management
Managing Osgood-Schlatter’s Disease
Diagnosis Of Osgood-Schlatter’s Disease
Osgood-Schlatter’s disease is mainly diagnosed by clinical presentation, meaning the presenting symptoms and physical examination of the child are usually enough to hone in on an accurate diagnosis, without the need for any radiological investigations. However, in saying that the use of additional tests, such as an x-ray, ultrasound scan, or MRI may be used to rule out other possible causes of the symptoms if there is any ambiguity with making a diagnosis. An X-ray of the area if taken will show a small area of separation at the site of insertion of the patella tendon to the tibia
confirming Osgood-Schlatter’s disease (see our previous blog titled Osgood Schlatter’s Disease: Not Really A Disease for a brief explanation of local anatomy).
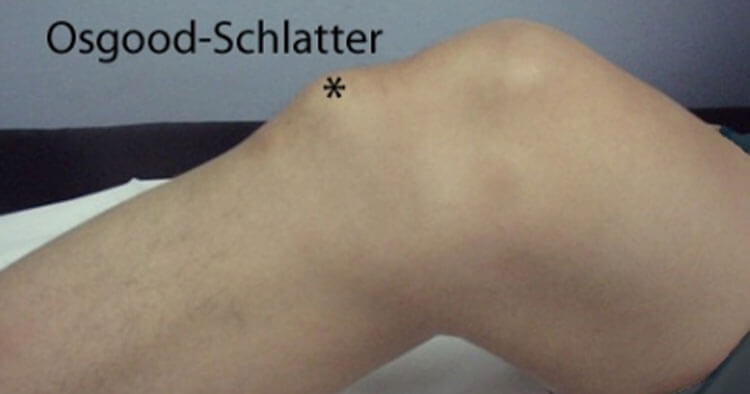
What Causes That Bump On The Front Of The Knee?
Your quadriceps muscles are joined to the tibial tuberosity vai the patella tendon. During bone growth, in Osgood-Schlatter’s disease the point where the tendon attaches to the shin bone becomes inflamed and micro-fractures occur at the bone. The body repairs these fractures by laying down extra bone tissue, with the end result of this being a larger than normal bump at the tibial tuberosity. The bump on the front of the knee is a pretty tell tale sign of the condition and in the acute phase this bump is typically very tender to palpation or knocking the area. The bump will generally remain through adult years but the sensitivity to pressure on the area subsides and it because just a cosmetic issue more than anything.
I Think My Child Has Osgood-Schlatter’s Disease, What Should I Do?
Firstly it is worth mentioning that this is not anything to be worried it is self limiting and given time your child will “grow” out of it and frequently all that is required is some activity modification to unload the area for a period of time to allow the pain to subside or calm down to a manageable level. If you suspect Osgood-Schlatter’s then:
- taking your child to their GP is a good starting point, they can order any appropriate imaging deemed necessary, offer advice and then refer on accordingly.
- you may prefer to take your child straight to see a physiotherapist, this is also a good option as frequently imaging is not necessary, your physio can always advise otherwise if they feel any imaging is appropriate.
The Management Of Osgood-Schlatter’s Disease
The cause with this syndrome is the excessive and repetitive stress placed on the growth plate at the insertion of the patella tendon. Children are more prone to this problem when they are going through a growth spurt and the muscle/tendon development verses the growth of the local bone tissue is out of balance. High levels of activity around significant growth periods could be avoided to help keep the condition at bay.
Ultimately symptomatic treatment is the key in managing the condition, painful activities should be avoided during an exacerbation of the condition. Treatment is directed at managing, not curing, as the syndrome itself is self limiting and the child will usually grow out of it. During a period of exacerbation the severity of the pain can be quite limiting, impacting participation/enjoyment of many sports and activities. Some of the techniques and approaches physiotherapists can use to help control the pain and aid returning the child back to their normal level of activity include:
- A RICE regime when the knee/s are painful.
- Recognizing the painful triggers and reducing them when necessary. Activity modification or relative rest – completely avoiding activities that are painful for at least a couple of weeks followed by gradual return to activity, guided by symptoms.
- Occasionally it may be necessary to rest the knee via a brace/splint when the pain is very severe, to enforce a brief period of rest.
- Even more rarely and only when growth has finished, if a small loose body remains in the tendon this may need to be surgically removed if symptoms persist.
- Improving the child’s pelvic and core stability as well as their lower limb stability can aid in improving biomechanics and assist in unloading the painful area.
- Improving the alignment and lower limb biomechanics again through strengthening, footwear changes, again this can aid in somewhat unloading the painful area.
- Muscle stretching of tight structures in and around the lower limb can prove beneficial in some children.
- The use of taping, padding, or braces in an attempt to take pressure off the painful area is another useful technique.
- Likewise the use of impact orthotics may aid in load transference reducing the forces transmitted to the painful area.
What Is The Long Term Prognosis
Osgood-Schlatter’s disease is a self limiting syndrome and usually resolves by itself within 12 months. However, with some children the knee may remain uncomfortable until their growth development finishes. The pain usually resolves by itself with a period of activity modification and a combination of the above mentioned treatment approaches. Being a self limiting syndrome, the child will grow out of it with little, if any complications, however it is still a good idea to see your local physiotherapist to get some help in managing the condition and get them back to doing what they love sooner.
Disclaimer: Sydney Physio Clinic does not endorse any treatments, procedures, products mentioned. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific advice or assistance on Managing Osgood-Schlatter’s Disease should consult his or her general practitioner, physiotherapist or otherwise appropriately skilled practitioner.